A breakdown of 2024 split or shared visits
Let’s break down the concept of split (or shared) visits and explore any recent developments associated with this practice.
Split or shared visits refer to Evaluation and Management (E/M) encounters where both a physician and a qualified healthcare professional (QHP) from the same group practice participate in providing care to a patient in a facility setting. This collaborative approach allows for comprehensive patient care, leveraging the expertise of both the physician and the QHP.
In these scenarios, it’s important to note that the billing method known as “incident to” is not applicable. “Incident to” billing typically involves services provided by non-physician practitioners under the supervision of a physician, but in split visits, both professionals are actively involved in delivering the care.
One significant aspect of split visits is the reimbursement structure under Medicare. Physicians receive 100 percent of the Medicare Fee Schedule (MFS) rate for their services during these encounters. In contrast, QHPs are reimbursed at 85 percent of the Physician Payment Schedule rate.
Here’s where the recent changes come into play: In response to advocacy efforts by organized medicine, the Centers for Medicare & Medicaid Services (CMS) is proposing a one-year delay in implementing a policy change. This change was set to require a physician to spend more than half of the total time during a split or shared E/M visit with the patient to be eligible to bill for the service. The policy, initially planned to take effect in 2023, was paused due to concerns about its potential disruption of team-based care and its impact on the way healthcare is delivered in a facility setting, as it did not account for the medical decision-making by the physician.
The long-standing CMS policy had been that a physician could bill for a split or shared visit if they performed a substantive portion of the encounter. This substance could be defined in several ways: It could be in terms of the history obtained from the patient, the physical examination conducted, the medical decision-making involved, or the physician spending more than half of the total time with the patient.
As we move into calendar year 2024, physicians will still be able to bill for split or shared visits based on the existing definition of a “substantive portion.” However, it’s worth noting that CMS has expressed its intention to seek additional guidance from the Current Procedural Terminology (CPT) Editorial Panel. The CPT Editorial Panel has already approved revisions to the E/M guidelines that provide further definition, and this information will be available in the CPT 2024 publication. This guidance will likely clarify how split or shared visits should be documented and billed in the future.
Here is a table form of the new 2024 changes.
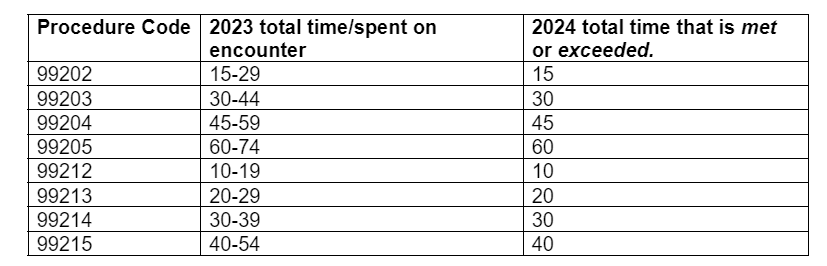
In medical billing, it’s important to stay updated on such policy changes and to be prepared to adapt billing practices in response to evolving regulations, which can significantly impact reimbursement and coding procedures.
